Breakthrough brain-Computer Interface Brings New Solutions for Resistant Depression
Transforming Depression Treatment with Next-generation Neural Technology
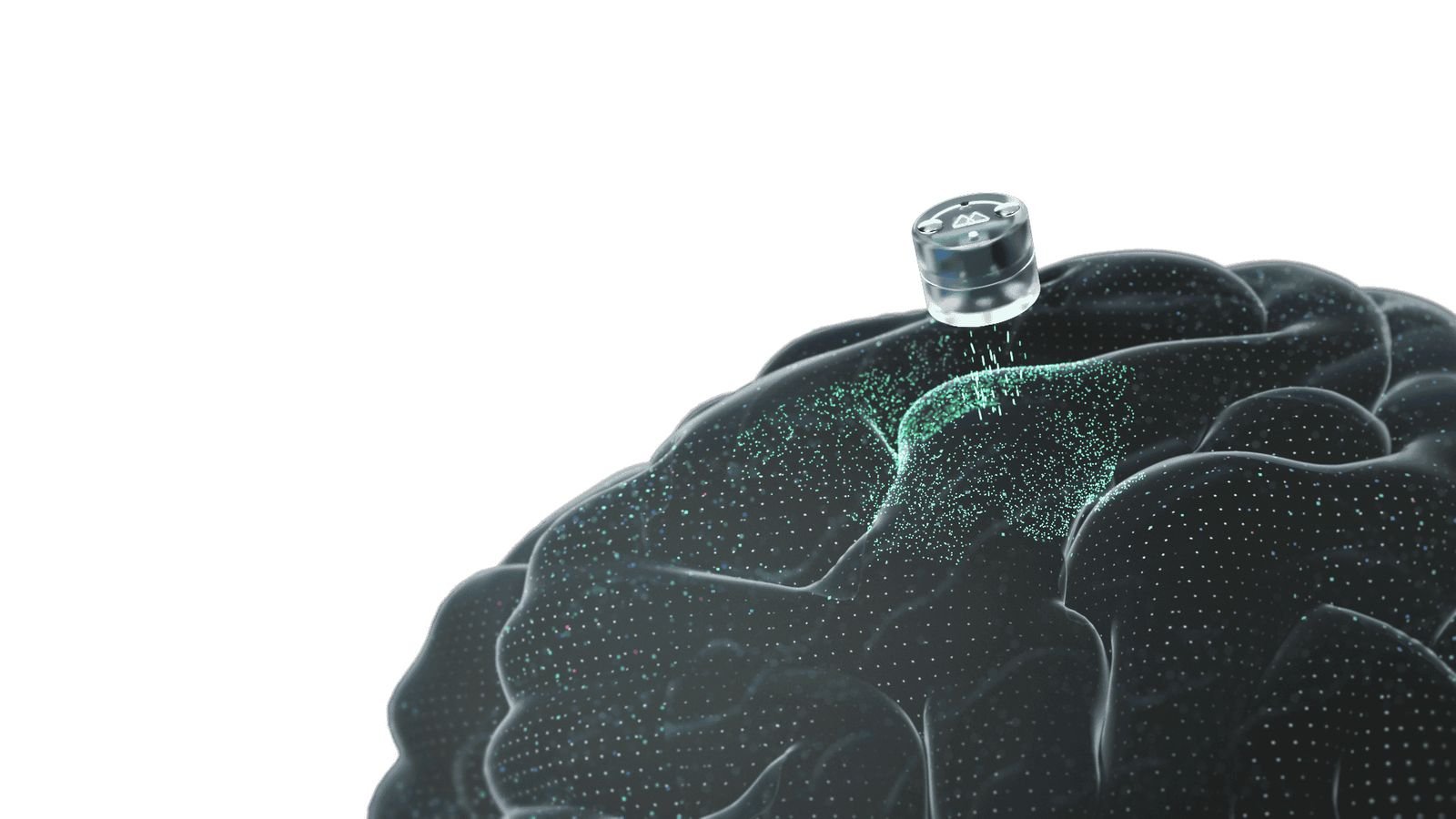
A novel brain-computer interface (BCI) device is set to revolutionize care for patients battling severe depression that remains unresponsive to traditional therapies. Motif Neurotech, a Houston-based startup founded in 2022, has secured FDA approval to commence human trials of its miniature brain implant-comparable in size to a blueberry-that delivers precise electrical stimulation directly within the cranial cavity.
Activating Key Brain Networks to Alleviate Major depressive Disorder
The implant is carefully placed just above the dura mater, the protective layer surrounding the brain. It targets the central executive network (CEN), a vital neural circuit involved in high-level cognitive functions such as emotional regulation and decision-making. Studies reveal that this network shows diminished activity in individuals diagnosed with major depressive disorder (MDD). By delivering targeted electrical pulses, Motif’s technology aims to reactivate this underperforming region and reduce depressive symptoms effectively.
Convenient at-Home Neurostimulation Empowers Patients
This innovative device allows patients to receive therapeutic stimulation from home through wireless transmission embedded within a specially designed cap resembling a baseball hat.The cap wirelessly powers the implant and controls treatment settings, enabling users to undergo multiple daily sessions lasting between 10 and 20 minutes during initial therapy stages. This approach encourages neuroplasticity-the brain’s capacity for self-repair-strengthening connectivity within mood-regulating networks over time.
Ancient Context: Evolution of Electrical Therapies for Depression
The use of electrical stimulation as an antidepressant dates back nearly one hundred years. Electroconvulsive therapy (ECT), introduced in the early 20th century, remains an option today but involves significant side effects and requires anesthesia. Deep brain stimulation (DBS), which implants electrodes deep into specific regions of the brain surgically, has been explored experimentally but faces regulatory hurdles due to its invasive nature and associated risks.
More recent innovations like transcranial magnetic stimulation (TMS) provide non-invasive alternatives by applying magnetic fields externally; though, TMS necessitates frequent clinical visits-frequently enough five times per week over six weeks-to achieve therapeutic benefits.
Tackling Treatment-Resistant Depression: A Growing Public Health Challenge
In the United States alone, approximately nine million adults receive treatment annually for major depressive disorder; about one-third experience treatment-resistant depression where symptoms persist despite multiple medication attempts. This underscores an urgent need for novel interventions that offer effective relief without requiring prolonged hospitalization or invasive procedures.
Simplified Implantation Process Powered by Cutting-edge Magnetoelectric Technology
The implantation procedure lasts roughly twenty minutes on an outpatient basis without necessitating full neurosurgery-a notable betterment compared with traditional DBS techniques. Utilizing magnetoelectric technology developed at Rice university by cofounder Jacob Robinson, this system wirelessly charges via external wearable devices while delivering finely tuned electrical impulses customized according to individual patient requirements.
clinical Trial Goals and Future Innovations on the Horizon
- The primary focus is ensuring safety throughout a year-long post-implantation monitoring period;
- Secondary objectives include assessing reductions in depressive symptoms alongside improvements in anxiety levels, cognitive function, and overall quality of life;
- The initial study will enroll around ten participants who have not responded adequately to existing treatments;
- Future iterations aim at integrating real-time neural activity monitoring capabilities into devices allowing personalized adjustments based on continuous feedback from patients’ brains;
“Unlike diabetes management where blood sugar provides objective data points,” explains Robinson’s vision involves generating continuous neurological data streams so clinicians can tailor psychiatric treatments more precisely.”
A Paradigm Shift: Personalized Psychiatry Through Advanced Brain Monitoring Devices
This cutting-edge approach marks progress toward precision mental health care where therapies adapt dynamically rather than relying solely on subjective symptom descriptions or trial-and-error medication strategies. As neuroscience advances hand-in-hand with miniaturized electronics seamlessly interfacing with human physiology, technologies like Motif’s BCI hold promise for redefining how millions worldwide manage chronic mental health conditions such as depression.