Transforming Vaccine Guidelines adn Accessibility in the United States
Emerging Trends in Covid-19 Vaccination Policies
the trajectory of Covid-19 vaccine distribution and insurance coverage across the U.S. faces uncertainty as a newly restructured Advisory Committee on Immunization Practices (ACIP) convenes this week in Atlanta. This committee, recently reorganized by Health and Human Services Secretary Robert F. Kennedy Jr., now includes members who express critical perspectives on vaccines, raising concerns about potential shifts to established immunization protocols.
Among the key agenda items are updated recommendations for Covid vaccines alongside childhood immunizations such as hepatitis B and the combined measles, mumps, rubella, and varicella (MMRV) vaccine. These decisions hold significant influence because they determine which vaccines insurance companies must cover without cost-sharing under federal mandates.
Childhood Vaccination Guidelines Under Review: Hepatitis B & MMRV
the ACIP is considering revising longstanding guidance that newborns receive a hepatitis B vaccine dose within 24 hours of birth-a practice credited with reducing acute pediatric infections by over 99% as its introduction in 1991. Globally, timely management of this vaccine has prevented an estimated 38 million deaths among children born between 2000 and 2030 across nearly 100 low- and middle-income countries.
Current discussions suggest delaying this initial dose until age four-a proposal met with strong opposition from many health experts who emphasize that early vaccination is crucial to prevent mother-to-child transmission at birth when infants face their highest risk for chronic infection leading to liver cancer later in life.
The committee may also reconsider recommendations regarding the MMRV combination shot versus separate doses during early childhood due to concerns about increased fever-related seizures among toddlers aged one to two years receiving the combined vaccine. Even though CDC data estimate approximately a 5% risk rate for these generally benign seizures under age four with MMRV use, altering schedules could intensify parental hesitancy amid rising measles outbreaks-the highest reported as elimination was declared decades ago.
Insurance Coverage Amidst Policy Shifts
A coalition representing over 200 million insured Americans-including major plans like Blue Cross Blue Shield affiliates and Humana-has committed to continuing coverage for all currently recommended vaccines such as updated Covid-19 boosters and influenza shots irrespective of forthcoming ACIP changes. However,some large insurers like UnitedHealthcare remain outside this agreement.
The Role of Government Programs in Ensuring Vaccine Access
Approximately half of U.S. children benefit from government initiatives like the vaccines for Children program that provides free immunizations aligned with official guidelines; Medicare and Medicaid similarly require no-cost coverage for approved vaccines while private insurers must comply under laws such as the Affordable Care Act-provided those vaccinations retain endorsement by ACIP’s current framework.
Any weakening or removal of routine endorsements risks pushing families toward out-of-pocket expenses that can delay essential vaccinations critical for maintaining community immunity against preventable diseases.
Divergent State-Level Policies Threaten Equitable Access
If federal recommendations become more restrictive or ambiguous following ACIP’s votes this week, states may respond unevenly-potentially creating fragmented access nationwide. Several West Coast states including California have proactively issued unified guidance encouraging all adults and children concerned about respiratory illnesses during fall-winter seasons to receive recommended vaccinations without prescription requirements at pharmacies.
Similarly, Democratic-led states such as Illinois and North Carolina have enacted measures facilitating pharmacy-based access without doctor orders; however Republican-led states often still mandate prescriptions before administering Covid shots or other immunizations outside clinical settings-a disparity disproportionately impacting rural populations where healthcare resources are limited.
Public Health Implications of Restrictive Recommendations
If ACIP narrows or delays vaccination guidelines during peak respiratory virus season-which now sees record hospitalizations due to influenza variants alongside persistent SARS-CoV-2 strains-it could exacerbate declining vaccination rates especially among healthy adults, children, and rural residents facing additional barriers obtaining prescriptions or locating vaccination sites.
“Limiting broad access at critical times risks increasing vulnerability to outbreaks,” warns public health expert Neil Maniar from Northeastern University.
Navigating Scientific Consensus Versus Controversy Around mRNA Vaccines
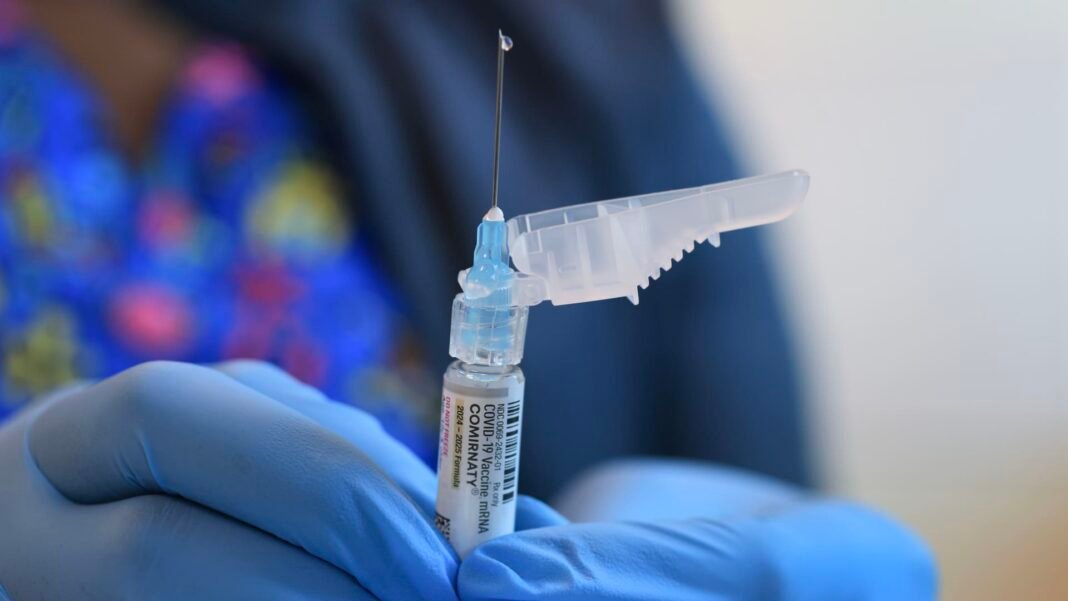
An extensive body of evidence confirms that mRNA-based covid-19 vaccines developed by Pfizer-BioNTech (Comirnaty) and Moderna remain safe-with serious adverse events being exceedingly rare even after billions administered worldwide through mid-2024-and studies estimate these vaccines have saved over two million lives globally since late 2020 rollout began.
Despite overwhelming data supporting safety profiles-including transient myocarditis cases primarily affecting young males post-vaccination but resolving without lasting harm-some ACIP members have voiced unsubstantiated claims linking these vaccines with severe adverse effects among younger populations.
This discord fuels public confusion regarding trustworthy sources on vaccine safety amid ongoing pandemic waves driven by emerging variants posing continued threats especially toward vulnerable groups including elderly individuals or those with compromised immune systems prone to severe illness if unvaccinated.
Kawsar talaat, an international health professor at Johns Hopkins Bloomberg School emphasizes: “Conflicting messages undermine confidence making people less likely to adopt proven protective measures.”
Misinformation Risks Undermining public Trust Before Critical Decisions
Tensions surrounding upcoming votes include reports alleging pediatric deaths directly linked to Covid vaccinations based solely on unverified VAERS data submissions-a passive reporting system designed not for establishing causality but rather signal detection requiring rigorous follow-up investigations.
Such claims threaten scientific integrity when fabricated citations previously surfaced during advisory meetings undermine evidence-based policymaking processes vital during periods demanding clear communication grounded firmly in verified research rather than conjecture or politicized narratives.
With seasonal surges expected alongside persistent viral evolution necessitating accessible booster campaigns tailored per individual risk profiles based on robust clinical data interpretation-not ideological bias-the stakes remain exceptionally high going forward into winter months ahead.
The Road Ahead: Strengthening Immunization Efforts Across America
This pivotal juncture underscores how transformations within influential advisory bodies reverberate throughout healthcare delivery systems affecting millions’ ability-and willingness-to obtain lifesaving vaccinations against both longstanding infectious diseases like hepatitis B plus emerging threats exemplified by evolving SARS-CoV-2 variants circulating globally today.
Ensuring equitable distribution paired with clear science-driven policies remains essential amid shifting political landscapes shaping public health priorities nationwide into coming years marked increasingly by complex challenges requiring unified commitment toward prevention strategies proven effective repeatedly worldwide through decades-long successes combating infectious disease burdens via comprehensive immunization programs embraced universally across diverse populations regardless geography socioeconomic status demographics alike alike alike alike alike alike alike alike .